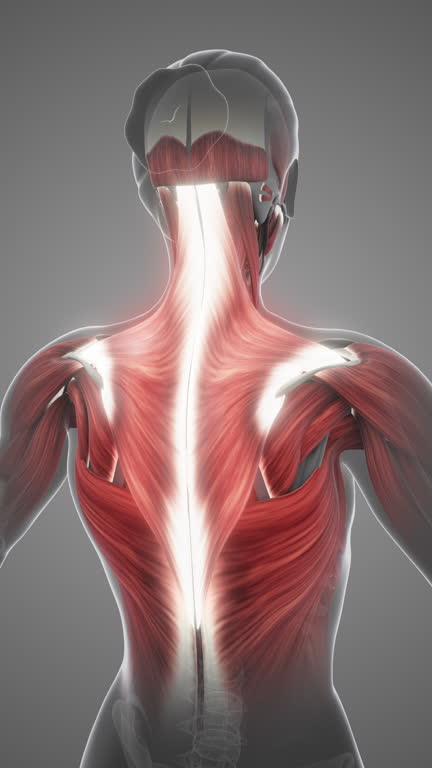
A stethoscope, a simple yet powerful diagnostic tool, can help healthcare professionals detect early signs of spinal cord compression. This condition occurs when pressure is applied to the spinal cord, potentially leading to pain, weakness, and even loss of function. While advanced imaging techniques like MRI scans are the gold standard for diagnosis, the stethoscope remains a reliable, non-invasive first step.
What Is Spinal Cord Compression?
Spinal cord compression happens when external forces press on the spinal cord. This pressure disrupts normal nerve function and can lead to severe symptoms. Common causes include:
- Herniated discs: When the cushioning discs between vertebrae slip out of place.
- Tumors: Abnormal growths in or near the spinal cord.
- Injuries: Fractures or dislocations that impact the spinal column.
- Arthritis: Wear-and-tear damage causing bone spurs.
- Infections: Conditions like abscesses or tuberculosis in the spine.
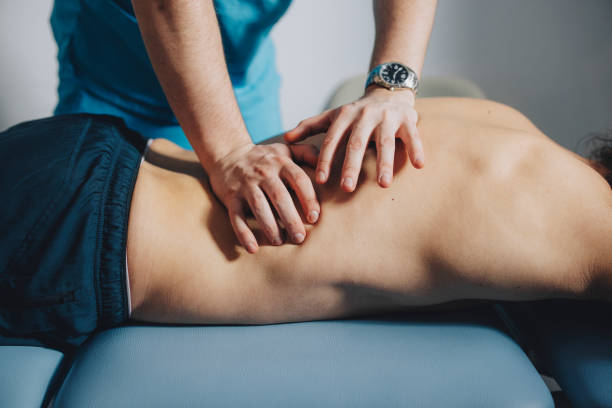
Symptoms can range from mild discomfort to serious nerve damage. Early detection and treatment are essential to prevent permanent disability.
How Does a Stethoscope Help?
Though typically associated with heart and lung examinations, the stethoscope is also useful in assessing spinal cord compression. Here’s how:
1. Detecting Changes in Blood Flow
A stethoscope can reveal abnormalities in blood flow near the spine. Restricted circulation, caused by compression, often produces unusual sounds such as:
- Bruits: A whooshing sound indicating turbulence in blood vessels.
- Muffled Flow: Suggests reduced blood supply, which may signal underlying compression.
2. Spotting Vascular Abnormalities
Certain spinal conditions impact nearby blood vessels. Listening for abnormal sounds around the spinal region can help identify vascular issues contributing to the compression.
3. Guiding Further Tests
While the stethoscope doesn’t provide a definitive diagnosis, it helps doctors decide if advanced imaging like an MRI or CT scan is necessary. It’s especially valuable for screening patients in clinical settings or during initial evaluations.
Common Tools and Methods for Spinal Cord Compression Assessment
Let’s break down the different tools doctors use to assess spinal cord compression, including the stethoscope:
| Method | What It Does | When It’s Used | Benefits | Limitations |
| Stethoscope | Detects abnormal blood flow and vascular sounds | Initial evaluation | Non-invasive, quick, cost-effective | Limited to vascular assessment |
| Physical Examination | Assesses reflexes, strength, and mobility | Early detection | Simple and inexpensive | Relies on patient cooperation |
| MRI Scan | Creates detailed spinal images | Confirming diagnosis | Highly accurate | Expensive, not always immediately available |
| CT Scan | Provides cross-sectional images of the spine | Identifying structural damage | Useful for hard tissue assessment | Higher radiation exposure |
| X-Ray | Identifies bone injuries or alignment issues | Quick overview of spinal structure | Widely available | Poor visualization of soft tissues |
The stethoscope, though less detailed than imaging tools, is often the first step in identifying potential problems.
What Are the Symptoms of Spinal Cord Compression?
Knowing when to seek medical help is crucial. Look out for these warning signs:
- Pain: Persistent pain in your neck, back, or legs that worsens with movement.
- Weakness: Difficulty moving or lifting objects.
- Numbness: Tingling or loss of sensation in your arms, hands, legs, or feet.
- Bladder/Bowel Issues: Difficulty controlling urination or bowel movements.
- Balance Problems: Trouble walking or maintaining balance.
If you notice these symptoms, it’s essential to consult a healthcare professional immediately.
The Role of the Stethoscope vs. Imaging Tests
While a stethoscope provides initial clues, advanced imaging methods are often required for a complete diagnosis. Here’s a deeper comparison:
- Stethoscope: Detects surface-level vascular abnormalities. Ideal for quick, preliminary checks.
- MRI: Offers a 3D view of the spinal cord and surrounding tissues. It’s best for pinpointing the exact cause of compression.
- CT Scan: Focuses on structural damage like fractures or bone spurs.
- Electromyography (EMG): Assesses nerve function and detects muscle damage caused by nerve issues.
Using these tools together provides a comprehensive understanding of spinal cord health.
When Should You See a Doctor?
Early intervention is vital. You should seek medical attention if you experience:

- Severe or worsening pain in your back or neck
- Numbness or tingling that doesn’t go away
- Loss of strength in your limbs
- Difficulty with coordination or balance
- Uncontrolled bladder or bowel movements
Prompt evaluation and treatment can prevent complications like permanent nerve damage or paralysis.
Treatments for Spinal Cord Compression
If spinal cord compression is diagnosed, treatment options vary based on severity. Common approaches include:
- Physical Therapy: Strengthening muscles to relieve pressure.
- Medications: Anti-inflammatory drugs to reduce swelling.
- Surgery: For severe cases, procedures like decompression surgery may be needed.
- Lifestyle Changes: Weight management and posture improvement to reduce stress on the spine.
Conclusion: Stethoscope Use in Spinal Cord Compression
The stethoscope plays a vital role in assessing spinal cord compression, helping doctors identify early signs of trouble. While it’s not a replacement for advanced imaging, it’s a quick, cost-effective tool for initial evaluations. If you notice symptoms like pain, weakness, or numbness, don’t ignore them. Seek medical advice right away to prevent long-term complications.
Understanding the tools and methods for spinal health can empower you to make informed decisions and take better care of your spine.