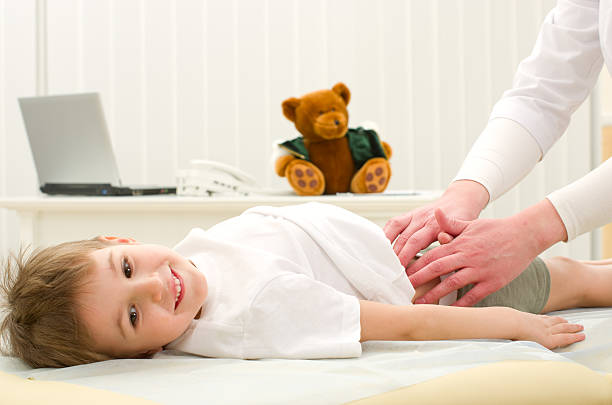
Abdominal pain in children is a frequent complaint that can signal anything from mild conditions to serious emergencies. This guide will help you assess the symptoms effectively, ensuring timely treatment. Let’s dive deeper into understanding the causes, evaluation, and management of pediatric abdominal pain.
Why Assessing Abdominal Pain in Children is Critical
Children often struggle to express what they feel, making abdominal pain challenging to diagnose. While it’s common for kids to experience stomachaches, you must determine whether it’s a minor issue or a sign of something more severe, like appendicitis or intestinal obstruction.
Understanding Pediatric Abdominal Pain
Types of Abdominal Pain

- Acute Pain: Starts suddenly and is often severe. Conditions like appendicitis or intestinal obstruction may cause this.
- Chronic Pain: This lasts for weeks or months, often related to functional gastrointestinal disorders.
- Recurrent Pain: Comes and goes, commonly linked to stress or dietary issues.
Common Causes
- Indigestion: This may result from overeating or eating spicy/greasy foods.
- Constipation: A prevalent issue due to insufficient fiber or water intake.
- Gastroenteritis: Caused by viral or bacterial infections, leading to diarrhea, vomiting, and fever.
- Appendicitis: A medical emergency characterized by sharp pain in the lower right abdomen.
- Food Allergies: Pain triggered after eating certain foods, accompanied by rashes or swelling.
The Best Approach to Abdominal Pain in Pediatrics
Step 1: Medical History
Ask specific questions to narrow down potential causes:
- Where is the pain located?
- When did it start, and is it constant or intermittent?
- Does anything improve or worsen the pain?
- Are there additional symptoms, like fever, vomiting, diarrhea, or weight loss?
Step 2: Physical Examination
Conduct a thorough but gentle exam to:
- Identify areas of tenderness or swelling.
- Check for signs of abdominal distension.
- Observe the child’s behavior, like guarding the abdomen or reluctance to move.
Step 3: Use Pediatric Abdominal Pain Guidelines
Pediatric abdominal pain guidelines provide a structured framework for diagnosis and management. These guidelines emphasize the importance of identifying red flags and choosing appropriate diagnostic tests based on symptoms.
Pediatric Abdominal Pain Red Flags
Some symptoms require immediate medical attention:
- Severe, persistent pain lasting over 2 hours.
- High fever with abdominal pain.
- Blood in vomit or stool.
- Distended abdomen.
- Sudden, sharp pain that worsens rapidly.
Ignoring these signs can lead to complications, such as perforated appendicitis or intestinal obstruction.
Pediatric Abdominal Pain Differential Diagnosis
Differentiating between possible causes is essential to provide the right care. Below is a detailed comparison:
| Condition | Key Symptoms | Diagnosis | Treatment |
| Appendicitis | Pain starts around the navel, and shifts to the lower right | Ultrasound or CT scan | Emergency surgery |
| Gastroenteritis | Diarrhea, vomiting, fever | Stool culture | Hydration, rest |
| Constipation | Hard stools, bloating | Abdominal X-ray | Dietary changes, laxatives |
| Food Allergies | Pain, rashes, swelling after eating | Allergy tests | Avoid triggers, antihistamines |
| Intestinal Obstruction | Severe bloating, vomiting, inability to pass stool | Imaging studies (X-ray/CT) | Surgery or decompression |
| Functional Abdominal Pain | No clear physical cause, stress-related | Exclusion of other conditions | Counseling, dietary modifications |
This table highlights the differences between conditions, helping you pinpoint the problem.
Diagnosing Acute Abdomen in Children
What is Acute Abdomen?
Acute abdomen refers to sudden, severe abdominal pain requiring immediate medical intervention. Conditions like appendicitis, perforated ulcers, or twisted intestines fall under this category.
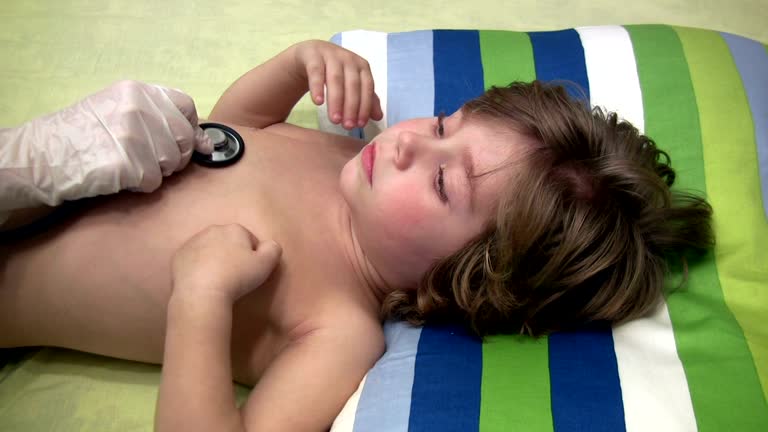
Diagnostic Tools
- Ultrasound: A safe, non-invasive method to detect organ issues.
- X-rays: Useful for detecting blockages or perforations.
- Blood Tests: Can reveal infections or inflammation.
Early diagnosis reduces the risk of complications and improves outcomes.
Pediatric Abdominal Pain in Emergency Medicine
When abdominal pain presents as an emergency, follow these steps:
- Stabilize the Patient: Ensure the child’s airway, breathing, and circulation are stable.
- Rapid Assessment: Identify life-threatening conditions using imaging or blood tests.
- Initiate Treatment: Administer pain relief, fluids, or antibiotics as needed.
- Decide on Surgery: For acute appendicitis or intestinal obstruction, prompt surgical intervention is critical.
Pediatric Abdominal Pain Treatment Options
Treatment varies depending on the diagnosis:
- Hydration: Essential for gastroenteritis or dehydration caused by vomiting.
- Dietary Adjustments: Increase fiber for constipation or eliminate trigger foods for allergies.
- Medication: Antacids for indigestion, laxatives for constipation, or antibiotics for infections.
- Surgery: Necessary for appendicitis, intestinal obstruction, or other emergencies.
How to Manage Recurrent or Chronic Abdominal Pain
For recurrent pain, focus on:
- Identifying stressors or triggers.
- Encouraging a balanced diet with plenty of water and fiber.
- Consulting a pediatrician for further evaluation.
Conclusion
Assessing abdominal pain in children involves understanding their symptoms, using pediatric abdominal pain guidelines, and recognizing red flags. Always take a systematic approach to identify the cause. Whether it’s a mild case of indigestion or a serious emergency like acute appendicitis, timely intervention is crucial.
By staying informed, you can make better decisions and provide the care children need. If the pain persists or severe symptoms occur, seek medical help immediately.